Screening for congenital heart disease in newborn babies is essential. Timely made diagnoses may make a difference between life and death and without a doubt, may contribute to better outcomes for an affected child.
There are three actions that will help in the detection of congenital heart disease in newborns after birth:
- observation of the baby’s behavior after birth (quality of breathing with and after feedings)
- physical examination (abnormal findings in respiratory and cardiovascular systems)
- pulse-oximetry or oximetry testing
What is Congenital Heart Disease and Critical Congenital Heart Disease?
The human heart is a very complicated organ consisting of four chambers (two atriums and two ventricles) with blood vessels coming in and out and blood flowing in a specific predetermined manner. Blood from the right ventricle flows into the pulmonary artery, which supplies blood to both lungs where the blood picks up oxygen. Then blood comes back to the left atrium and the left ventricle from where it is pushed out to the main artery called aorta and to all-important vital organs of the body. After releasing oxygen in tissues, blood comes back to the heart in veins and flows into the right atrium and the right ventricle again.
The fetus and newborn baby right after birth have functional and anatomical differences comparing to the anatomy of an adult person. Those differences compensate for the fact that lungs in a fetus are collapsed and not filled with air like after birth. The most crucial difference is the existence of ductus arteriosus, which is a vessel connecting the aorta and pulmonary artery.
Ductus arteriosus is supposed to get closed on its own soon after birth. In babies diagnosed with critical congenital heart disease, it is often desirable to keep that ductus arteriosus open using a medicine (Prostaglandin). If we allow for spontaneous closure of ductus arteriosus in a baby with undiagnosed critical congenital heart disease, that may lead to vascular collapse, severely low levels of oxygen in the body and even death.
Sometimes, the baby is born with structural and functional abnormalities of the heart affecting its oxygenation and overall health. That is a definition of congenital heart disease (CHD). Whenever congenital heart disease is severe and needs treatment with surgery or intra-cardiac catheter, such condition is called critical congenital heart disease (CCHD). Congenital heart disease occurs in 9-10 of every 1000 live births. Critical congenital heart disease is less frequent and occurs in approximately 2-3 of every 1000 live births (Source article).
Why early screening for Critical Congenital Heart Disease is so essential?
Human heart and circulation undergo many functional and anatomical changes within the first 72 hours after birth, making a diagnosis of any heart abnormalities after birth difficult. It is quite common that a baby with CHD is born looking very healthy and goes home two or three days later. Then, while at home within 1 or 2 weeks after discharge, the same baby is brought back to an emergency room in critical condition or even dies at home from CCHD.
If we recognize CCHD early, many babies who are affected can be treated successfully. Fortunately, the majority of congenital cardiac conditions can be treated with surgery. After diagnosis, we can start the medication to keep ductus arteriosus open – if indicated – and stabilize baby until necessary surgery or catheterization procedure can be done.
Over the last two decades, doctors tried to develop screening programs that could help them in the timely identification of babies with CCHD. CCHD Screening program should help us identify babies that have a high likelihood of having CCHD or CHD. Once we identify that group of babies, we can offer to do an ultrasound of the heart (also called Echo) to make the diagnosis of CCHD or exclude it with absolute certainty.
How can we identify babies with Critical Congenital Heart Disease after birth?
In some cases, a prenatal ultrasound performed during pregnancy can suggest the presence of significant congenital heart disease. However, many times, prenatal ultrasounds miss that diagnosis due to technical difficulties and specifics of fetal anatomy.
Screening for CCHD starts right after birth. By observing the baby’s behavior, skin color, breathing pattern, and quality of feeding, we may have some idea about well being of the baby. If the baby quickly gets tired while eating, has increased sweating or faster breathing rate at rest, or after the feeding, one should consider the possibility of CCHD. During the physical exam, doctors look for heart murmurs, blood pressure abnormalities, or skin color changes (pale, grey, bluish skin color may signify low oxygen levels in the blood due to heart condition).
In the last two decades, doctors started using an additional tool in screening for critical congenital heart disease. We realized that heart conditions lead to lower oxygen levels in the blood, and that can be detected using pulse oximeter monitors even before skin discoloration becomes apparent to our eyes. In other words, before skin appears pale, cyanotic, or bluish on our examinations, we can detect abnormal oxygenation levels in the blood using a special monitor.
How doctors screen for critical congenital heart disease using pulse oximetry?
Pulse oximetry tests are recommended for all healthy newborn babies before their discharge home and in most institutions are conducted between 24 and 48 hours of life. Testing is not done on sick neonates staying in NICU as they are likely to have conditions affecting oxygenation levels not originating in their heart. Also, all babies staying in NICU are closely monitored, and CCHD is unlikely to be missed.
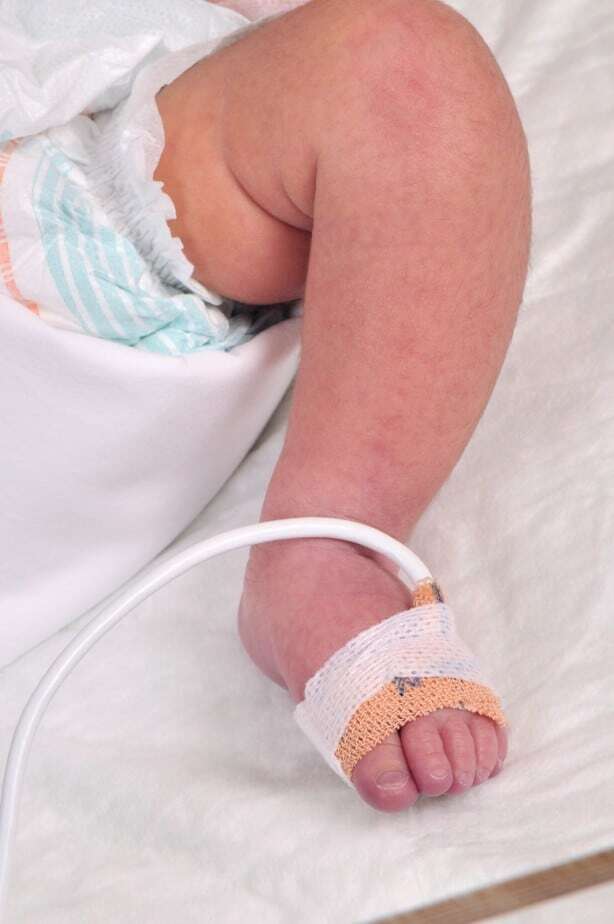
Picture on the left: pulse oximetry probe on the foot of the baby.
Pulse Oximetry testing is conducted by using a monitor (pulse oximeter or oximeter) that is capable of measuring the percentage of blood hemoglobin that is attached to oxygen. We take two measurements (they are called pre-ductal and post-ductal) by placing one probe on the right hand and another probe on the foot of the baby, and we get numerical results from both sites
Depending on the readings, we can determine if the baby passed this test, failed the test or that the test was inconclusive. The interpretation of the pulse oximetry screening test may differ depending on location and altitude. Below, I will present the most commonly used interpretation of oxygen saturation test:
- If both readings are equal or above 95% and the difference between the two readings is less than 3% – test is passed
- If both readings are within the range of 90% – 94% or the difference is more than 3% – the result is inconclusive, and one should repeat testing in an hour or proceed to evaluation with the ultrasound of the heart (Echo) or ask for urgent neonatology/cardiology consult
- If any of the readings are below 90%, one should urgently determine what is it due to. Usually, we will find abnormalities in the respiratory system or cardiovascular system that will need immediate treatment. Depending on the institution, neonatologist or pediatric cardiologist should be informed about such case as soon as possible.
One should remember that passing pulse oximetry screening does not exclude the presence of congenital heart conditions. If a baby shows symptoms and signs that might be associated with CCHD/CHD, that diagnosis should still be given serious consideration.
How effective is pulse oximetry as a screening for congenital heart disease?
Effectiveness of pulse oximetry screening for the detection of congenital heart disease will depend on a specific type of heart defect and frequency of its occurrence in each population or locale. This screening method aims at several primary and secondary targets.
Primary targets for CCHD screening:
- hypoplastic left heart
- pulmonary atresia
- truncus arteriosus
- tricuspid atresia
- tetralogy of Fallot
- TAPVR (total anomalous pulmonary venous return)
- dextroposition of great arteries
Secondary targets for CCHD screening:
- coarctation of the aorta
- double outlet ventricle
- Ebstein anomaly
- interrupted aortic arch
- single ventricle
The literature cites a sensitivity rate of 50%-75% for pulse oximetry in identifying babies with CCHD/CHD. That means that after conducting the test, still in 25%-50% of babies diagnosis will be missed. That’s why I want to emphasize again that passing pulse oximetry test does not exclude congenital heart disease (Source article).
However, pulse oximetry testing as a screening method is cheap, quick, easy, and cost-effective enough to be useful in the detection of at least 50% and possibly 75% of all babies affected by CCHD/CHD.
In summary:
Pulse oximetry is useful for screening of newborn babies soon after birth for congenital heart diseases. This screening method has been adopted in the USA and is also widely used in many other countries. It is effective due to ease of implementation and low cost. However, it misses some babies with CCHD/CHD, and parents and clinicians should remain vigilant for any signs of CHD even if the baby initially passed the oximetry screening test.
You may also be interested in reading my article: “What happens to a baby after birth in the hospital?” or another one on screening for hearing deficits here.
Disclaimer:
This article is only for general information purposes. It should not be viewed as any kind of medical advice. There is a chance that information here may be inaccurate. You should always discuss all health-related matters with your doctor before making any decisions that may affect your health or health of your family members.

