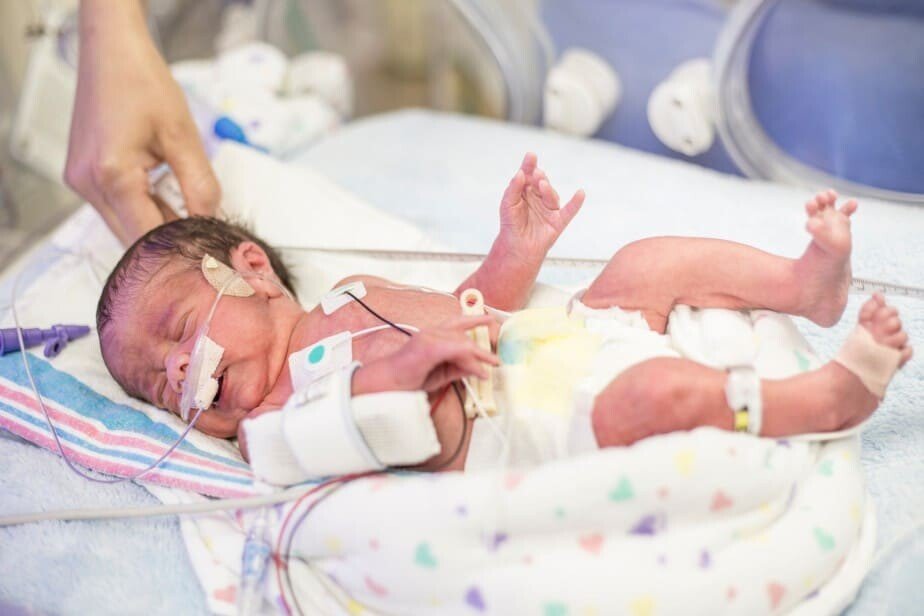
Full-term babies and late preterm babies may develop respiratory problems after birth. That, in turn, may lead to prolonged NICU stay and anxiety among the parents and family members. In this article, I will talk about the most common diagnosis causing those respiratory problems: Transient Tachypnea of the Newborn, which is also called Wet Lungs.
Transient Tachypnea of the Newborn (TTN) is a respiratory disease occurring in newborn babies due to insufficient or delayed clearance of the fluid from their lungs. The main symptoms after birth are a faster breathing rate and the need for supplementary oxygen. It almost always resolves within 48-72 hours after delivery.
Transient Tachypnea always needs to be differentiated from other respiratory problems affecting babies, such as Respiratory Distress Syndrome in preemies, Pneumonia, Developmental Disease, and others.
Why do babies develop TTN?
During pregnancy, the fetus is immersed in amniotic fluid. Fetal lungs produce fluid that plays a role in the lungs’ development. In preparation for the delivery and life out off the womb, three physiologic processes take place in a baby that facilitate the removal of fluid from the lungs.
- Production of the lung fluid is decreased in the last few days of the pregnancy.
- A significant amount of the fluid is absorbed from the lungs in the last few days during pregnancy and during labor.
- The remaining amount of the lung fluid is absorbed within the first hours after birth once the baby starts breathing.
In situations where these three steps in the fluid removal are inefficient, a baby may develop symptoms of Transient Tachypnea. Depending on the severity of these symptoms, some babies will be admitted to NICU and will receive supportive treatment (Source).
The following newborn babies are at higher risk of developing TTN:
- Delivery before completed 39 weeks of Gestational Age
- Delivery by cesarean section without preceding labor
- Large birth weight
- Male baby
- Maternal diabetes
- Mother having Asthma
- Multiples (twins, triplets, etc.)
The incidence of TTN among the full-term babies is estimated to be 5-6 cases per 1000 normal deliveries. Among late preterm babies, the frequency will be much higher.
What are the symptoms of TTN?
A typical presentation in TTN is that of otherwise healthy looking newborn that has increased respiratory rate and slightly decreased oxygen levels when using a pulse oximeter monitor to measure it.
Pulse-oximeter monitor is used to measure the amount of hemoglobin that is attached to oxygen. This non-invasive technique that takes its continuous reading from the probe placed on the baby’s hand or foot allows us indirectly evaluate oxygenation in a human body. The measurement is called oxygen saturation and is given in percentages. Adequate oxygen saturation in a healthy newborn baby should be above 92%.
The normal respiratory rate in newborns is below 60 per minute. Babies with TTN may breathe even more than 100 breaths per minute. Their breathing may be very shallow, and sometimes we also observe increased work of breathing. We talk about increased work of breathing when the baby is making noises while breathing (grunting), moving sides of its nose (nasal flaring), and pulling chest in just below the ribs (retractions) during respiratory effort.
How do we diagnose Transient Tachypnea of the Newborn (TTN)?
The diagnosis of TTN is a possibility whenever a well-appearing baby who is late preterm or full-term presents to us with an abnormally high respiratory rate (Source).
If the baby does not have oxygenation problems and disease is mild, we may decide only to observe the baby and not do any other diagnostic workup. However, if a baby requires oxygen or its condition is more severe, we will perform additional tests and evaluations to exclude other possible diagnoses:
- Blood gases – these tests allow us to determine the levels of oxygen and carbon dioxide in the blood. By doing blood gases, we can assess how severe the disease is and decide how aggressive we need to be treating it.
- Blood counts (CBC) and blood cultures – these tests are conducted to evaluate a baby for possible infections. Breathing problems can be the first presentation of infection. Therefore whenever a baby has more severe symptoms from the respiratory tract, we always consider treatment with antibiotics and evaluation for infectious disease. Complete Blood Count test gives us information on numbers of the white cells, which, when abnormal, may be suggestive of infection. Blood culture is a test in which we put a small amount of blood on a special sterile plate, and if overtime bacteria grow on it, it proves our earlier suspicion of an infectious disease.
- Chest X-ray – allows us to exclude certain lung diseases such as ruptured lungs, congenital abnormalities of the lungs or pneumonia. It is essential to point out that the appearance of the lungs on X-ray in TTN does not have characteristics allowing us to diagnose this condition with certainty. However still, X-ray may be very helpful to us whenever the baby has more severe symptoms of respiratory disease.
- Echo (Heart Ultrasound). Whenever we are not sure if a fast respiratory rate is caused by a problem in the lungs or abnormality in the heart, we can perform the Echo. Echo is an ultrasound study of the heart that allows us to determine the exact anatomy of the heart and rule out congenital heart disease.
How do we treat Transient Tachypnea of the Newborn?
The treatment that we will offer to a baby with TTN will depend on the severity of symptoms and how well the baby is coping with the condition. Some babies with mild symptoms do not need any treatment, and we can monitor them and wait for the resolution of symptoms without intervention.
For other sicker babies, depending on their condition, we may use the following treatments:
- NPO – Babies with fast respiratory rates are not allowed to breastfeed or bottle-feed due to the risk of aspiration. It is difficult for them to coordinate breathing, sucking, and swallowing when respiratory rate is above 60-70 breaths per minute. Whenever a baby’s respiratory rate is above those levels, we have two choices: give milk via a plastic tube directly into the stomach or stop feedings and start the baby on intravenous fluids.
- Antibiotics – Most babies with moderate and severe respiratory problems or persistent mild respiratory problems will be treated with antibiotics. After birth, we never know for sure if there is an ongoing infection in the baby, and we do not want to take chances that it is left untreated. We prefer performing evaluations for infection first, then starting babies on antibiotics. If the baby gets better and evaluation is negative, in most cases, we will stop medicines 48 hours later.
- Oxygen – Many babies with TTN have decreased oxygen levels in their bodies due to lower ability to absorb oxygen from their filled by the fluid lungs. As a result, they require an increased concentration of oxygen for breathing. Extra oxygen can be provided to them in different ways. If they do not have increased work of breathing, we can provide additional oxygen into the plastic box surrounding their head called Oxyhood. If a baby has an increased work of breathing, we can add supplementary oxygen into the circuit of nasal cannula, CPAP device, or a ventilator (see below for the explanations).
- Supporting respiratory efforts in a baby. If a baby has significantly increased work of breathing as described above, we have to support its efforts using various devices:
- Nasal cannula – is a small flexible plastic tube inserted in the baby’s nose that is providing a flow of air with additional oxygen. Nasal cannulas are used in milder cases of Transient Tachypnea.
- CPAP device – It is a device that provides additional pressure for the baby during the expiratory phase of its breathing efforts. Air with oxygen flows to the baby through special cannulas inserted in the nose or through the small mask placed around the baby’s nose. This type of respiratory support is used in babies with moderately increased work of breathing.
- Ventilator or Breathing Machine. Babies who have a severe form of TTN with abnormal levels of oxygen and carbon dioxide in their blood are placed on a ventilator. A ventilator is a machine that provides external artificial breaths for the baby through the plastic tube placed in the baby’s trachea (windpipe). If needed, supplementary oxygen is provided into the respiratory circuit as well. From my experience, I can tell you that it is rare for the baby with TTN to require treatment with the ventilator. Most babies with TTN who need respiratory support can be successfully treated with a nasal cannula or CPAP device.
The prognosis for the babies diagnosed with TTN
The prognosis for recovery from TTN is excellent. As I explained in my introduction, TTN is a condition of delayed adaptation to life outside of the womb after birth. The natural physiologic mechanisms will kick in soon after birth, and fluid will be absorbed and removed from the lungs. Baby will recover fully within 48-72 hrs.
If the baby does not improve significantly within that time frame, the baby is likely affected by another pathologic condition, not TTN.
In very rare situations, a baby may develop complications. Some babies, particularly those who required treatment with a CPAP device or ventilator may develop air leaks (rupture of the small portion of the lung). Also, some babies may acquire infections associated with the use of central lines and various types of catheters.
What questions you may want to ask if your baby has TTN and is staying in NICU?
- How severe is TTN in my baby?
- Are you sure that my baby is having TTN and not other diagnoses?
- Is the hospital equipped well and certified to treat my baby with all respiratory support needed, or should my baby be transferred to a higher level of care hospital?
- How are you planning to treat my baby?
- Can I still hold my baby?
- Can I provide breast milk for my baby?
- What do you think, how long will my baby need to stay in NICU and in the hospital?
If you would like to learn more about the Neonatal Intensive Care Unit, you can find my article about NICU here.
If your baby is born prematurely and having respiratory problems you should read my article on Respiratory Distress Syndrome as well.
Disclaimer:
This article is only for general information purposes. It should not be viewed as any medical advice. There is a chance that information here may be inaccurate. It would be best if you always discussed all health-related matters with your doctor before making any decisions that may affect your health or health of your family members.