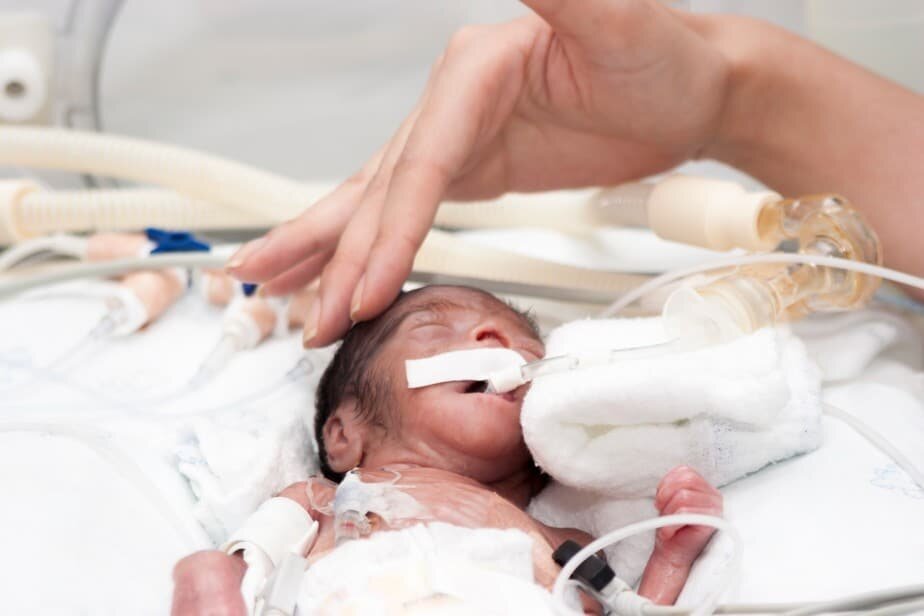
Respiratory Distress Syndrome or RDS is a lung disease occurring mostly in premature babies due to lung immaturity and surfactant deficiency.
Introduction, Definition, and What not to confuse it with?
RDS is a diagnosis given to babies with respiratory symptoms who have anatomical and chemical lung immaturity (chemical immaturity is due to surfactant deficiency in the baby’s lungs).
The majority of newborns with RDS are premature babies. However, some early-term babies and full-term newborns rarely may also be affected. Among more mature babies, newborns delivered by mothers who had diabetes during their pregnancy will have a higher risk of developing respiratory distress syndrome.
Lungs of the fetus undergo maturation process in utero that involves growing number of bronchial tree branches and increasing the production of a chemical called surfactant. An increase in the number of airways and alveoli (alveoli are tiny air bubbles in our lungs where oxygen – CO2 gas exchange takes place) contributes to increasing the surface area of gas exchange in our lungs. That process continues until birth and beyond.
Surfactant is a chemical being produced in our lungs and lining the alveoli. Its role is to prevent alveoli from collapsing. In other words, a surfactant is necessary for our lungs to function properly.
When a baby does not have enough airways, the gas exchange surface area is inadequate, the amount of surfactant is low, and the surfactant is malfunctioning; such a baby will develop respiratory distress syndrome after birth.
RDS can develop in any baby that is born prematurely; however, sometimes it may be due to genetic condition. Only a minority of babies with RDS have a genetic condition that affects the production of the surfactant, but cases like that will usually have a very severe clinical course.
In the past, RDS used to be called Hyaline Membrane Disease (HMD) or premature lung disease.
Some doctors use other terms to describe respiratory problems in newborn babies that should not be confused with respiratory distress syndrome or RDS. Sometimes we use term respiratory distress to indicate that the baby has a respiratory problem. Still, unless we say respiratory distress syndrome, it does not mean that it is due to immaturity of the lungs.
How common is Respiratory Distress Syndrome in premature babies?
The strongest risk factors for RDS are low gestational age at birth and low birth weight. Additional risk factors are maternal diabetes and hypoxia (low oxygen levels in the fetus before the delivery). The RDS is also more frequent among male babies.
95% to 98% of babies born at 22-24 weeks of gestation will have respiratory distress syndrome. 25%-50% of babies born at 28 – 32 weeks of gestation will have RDS.
The incidence of RDS drops down to 5% at 34 weeks of gestational age and to only 1% at 37 weeks of gestational age. Although it is uncommon for babies born at more than 37 weeks to have respiratory distress syndrome, it is not impossible.
Can RDS be prevented?
There are two ways to prevent or modify the course of Respiratory Distress Syndrome.
Preventing premature birth or at least delaying it is the best way to decrease the incidence and severity of RDS. Having regular prenatal care, proper nutrition, and life habits; all contribute to healthier fetus and pregnancy. In addition, there are some medications (called tocolytics) that can be given to slow down contractions and progression of labor.
If a mother is already in premature labor or threatened early labor, the administration of steroids to the mother (Bethametasone) can significantly increase the maturity of fetal lungs and decrease the incidence and severity of respiratory distress syndrome in a premature newborn baby (Source article).
There are several positive outcomes for the baby If at least 24-48 hours pass between administration of maternal steroids and delivery of the baby:
- the decrease in neonatal mortality
- decreased incidence and severity of RDS
- reduction in the incidence of intra-ventricular hemorrhage (bleeding in the brain)
Steroids may affect maternal blood pressure and glucose levels; however, more severe side effects are rare. Concerns about the possibility of an increase in infections in mothers or their babies have been unfounded.
Effects of repeated courses of steroids on premature babies’ long term outcomes such as neurodevelopment are still debated. Therefore, we need to be cautious if we want to offer 2nd or 3rd round of steroids to mother who returns 2 or 3 weeks later again in premature labor and has not delivered before.
What are the symptoms of RDS in preemies?
Symptoms in babies with Respiratory Distress Syndrome are non-specific. It means those same symptoms can occur in other respiratory problems that newborns have.
Symptoms in newborn babies with breathing problems:
- increased respiratory rate (also called tachypnea)
- grunting (expiratory noise while a baby is breathing)
- nasal flaring (movements of sides of the nose while a baby is breathing)
- retractions (sinking movements of chest wall below lower ribs when a baby is inhaling air)
- decreased breath sounds when doctors listen to the lungs
- reduced levels of oxygen and increased levels of carbon dioxide in blood tests (such test is called blood gas)
- decreased hemoglobin saturation (can be seen on the bedside monitor, normal values are considered to be above 92%
If the baby has increased respiratory rate and also presents with nasal flaring, grunting, and retractions, we often say that the baby has “increased work of breathing.”
How is the diagnosis of Respiratory Distress Syndrome (RDS) made?
Diagnosis of Respiratory Distress Syndrome in a newborn baby is always presumptive. There is no single test that could confirm the diagnosis of this condition with 100% certainty at the bedside.
Whenever we have a premature baby or baby with additional risks for RDS with respiratory symptoms, we presume that the baby has RDS. Additionally, a chest x-ray may be somewhat helpful but also is not diagnostic, since other conditions (GBS pneumonia) can mimic RDS on chest x-ray. Clinical course consistent with RDS is of the disease that shows symptoms soon after birth, and in the first few days, symptoms will be gradually getting worse if not treated.
How do we evaluate the severity of RDS in babies?
Evaluation of the severity of Respiratory Distress Syndrome relies on:
- clinical observation and examination
- chest x-ray
- blood gases and oxygen saturation levels
While conducting an examination, we pay particular attention to the amount of oxygen needed by the baby and the amount of work of breathing: severity of retractions and respiratory rate. Need for additional oxygen over 50%, deep subcostal chest retractions, and high respiratory rate of more than 100 per minute usually signify severe RDS.
On chest x-ray, severe RDS is defined by reduced lung expansion and poor aeration of the lung fields. If the doctor describes the lungs as entirely whited-out, that probably means severe RDS.
Blood gases allow us to assess the efficiency of gas exchange taking place in the lungs and the evaluation of chemical-metabolic balance in the body. Low oxygen levels, high carbon dioxide levels, and acidosis mean more severe RDS in a baby.
Treatment of Respiratory Distress Syndrome
The treatment of RDS is mostly symptomatic, and with one exception described below, it is not-specific for RDS. We want to support the baby with different measures to maintain the physiologic functions of the body without disturbing the baby too much. That way, we allow natural processes to take place, and we promote self-healing of the lungs.
After birth, the baby’s lungs accelerate the maturation process. Eventually, the lungs reach the level when the baby will be breathing more comfortably and will not need so much oxygen for breathing as right after birth.
Depending on the severity of Respiratory Distress Syndrome, we can use one or several of the measures described below:
- NPO – no feedings
- IV fluids to maintain proper hydration
- Antibiotics – many times we can not exclude infection contributing to baby’s respiratory problems
- Supplementary oxygen: starting from 21% up to 100% oxygen (Room air with which we breath has only 21% of oxygen)
- Supporting work of breathing with Nasal Cannula, CPAP device or ventilator (ventilator machine provides artificial/external breathing for the baby)
- Blood transfusions if a baby is severely anemic
- Blood pressure support with medications if a baby is hypotensive (Hypotension = low blood pressure)
- Surfactant administration
Surfactant is the only medication that is specific to the treatment of RDS. Surfactant got introduced to our treatment repertoire in early1990, and now, I can say that it is an essential medication in neonatology.
Surfactant is a complex substance that contains phospholipids and unique types of proteins. It can be produced synthetically or obtained from natural preparations of extracts from calf lung lavage, minced bovine, or porcine lungs. The latter, natural forms of surfactants, are more popular, better understood, and known to us, and probably more effective in the treatment of Respiratory Distress Syndrome.
Surfactant is a liquid medication that needs to be administered directly into the baby’s lungs. At this time, it can only be done by inserting a catheter or breathing tube (ET tube) into the baby’s trachea (windpipe) and injecting a surfactant down into the tube (Source article).
In the future, we might be able to provide surfactant by nebulization in aerosolized form but this method is still under development and in research trials.
Outcomes and prognosis of RDS in premature babies
In most cases, Respiratory Distress Syndrome improves after several days, and the baby can grow out of this condition. Obviously, the most affected babies and most premature babies may have many other medical problems contributing to their failure to recover.
In micro-preemies and extremely premature babies, RDS may evolve into chronic lung disease, also known as BPD. In the acute phase, a small group of babies may develop air leaks or pneumothorax. In pneumothorax, a tiny portion of lung ruptures and air leaks out from the lung into the space between the internal chest wall and the lung. That, in turn, causes compression of the lungs and prevents the lungs from expanding and functioning properly.
Pneumothorax can be dangerous and develops suddenly, resulting in acute deterioration of the clinical condition. The good news is that if recognized promptly, pneumothorax is treatable. The baby can still completely recover from pneumothorax and RDS.
In Summary:
Respiratory Distress Syndrome is a pulmonary condition occurring mostly in premature babies due to lung immaturity and surfactant deficiency. Treatment is primarily non-specific and supportive. Surfactant is the medication that can be administered to patients with moderate or severe RDS. Prevention and modification of severity of RDS rely on the prevention of premature labor and birth, and administration of steroids to mothers in early labor.
If you have a premature baby born before 32 weeks receiving treatment in the NICU right now, I encourage you to explore my book “Babies Born Early“
If you are interested to learn about the NICU; levels of care, people and equipment used there, click here.
Disclaimer:
This article is only for general information purposes. It should not be viewed as any medical advice. There is a chance that information here may be inaccurate. It would be best if you always discussed all health-related matters with your doctor before making any decisions that may affect your health or health of your family members.