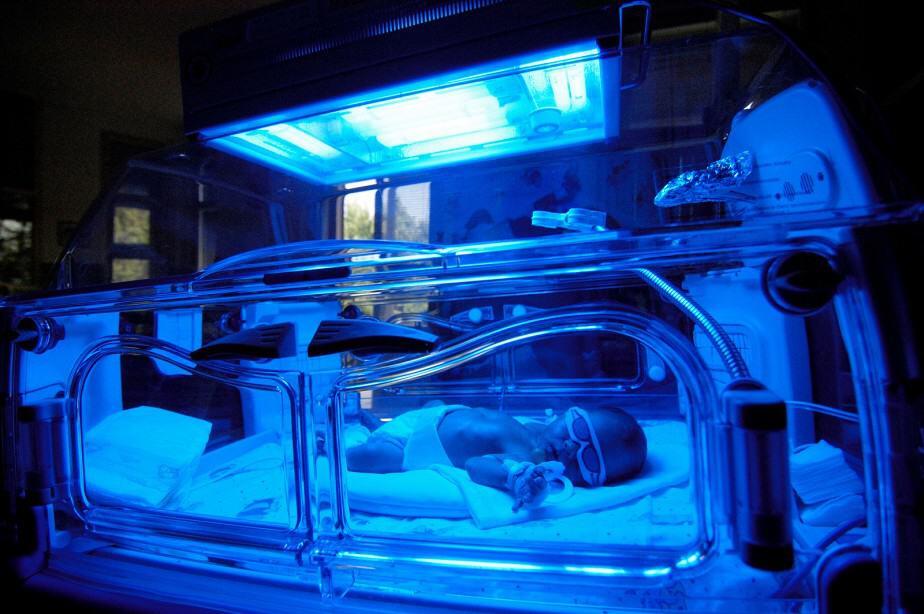
Jaundice is a prevalent condition among newborn babies, both full-term and premature ones. It often results in additional blood tests, the need for therapy, and delayed discharge home. Lack of knowledge about this condition is a source of anxiety among parents and families.
This particular article is very comprehensive and may be too difficult for some readers, especially if you have less than high school education. However, given the importance of this topic, I wanted to provide you with a complete resource.
Definition of jaundice. What causes newborn jaundice disease?
Jaundice is a term used to describe the presence of yellow skin color in a baby. Jaundice is caused by the accumulation of bilirubin in the skin. Bilirubin is a naturally occurring chemical in our body. Jaundice is due to increased bilirubin levels, so doctors call it Hyperbilirubinemia. Bilirubin levels depend on its production, elimination, and reabsorption.
Bilirubin is produced during the break down of red blood cells. Then it circulates in the body. Some of it is transported to the liver where it undergoes transformation called conjugation, allowing it to be excreted into the bowel loops with the bile and then excreted with the stool.
During passage through the gut, some of the bilirubin gets reabsorbed into the circulation again. Four processes can influence and lead to significant jaundice in the newborn baby:
- Increased production of bilirubin
- Decreased elimination of bilirubin
- Increase reabsorption of bilirubin from the gut
- Disorders of excretion from the liver
Jaundice due to increased production of bilirubin
Red blood cells have a limited life span. In adults, they live 120 days but in newborns much less. Conditions that shorten life span of the red blood cells will be contributing to increased bilirubin levels.
Isoimmunization
When there is a difference between blood types of the baby and the mother, there is a chance that maternal antibodies enter the baby’s circulation and will increase the destruction of baby’s red blood cells, thus contributing to higher bilirubin load. The ABO incompatibility, when the mother is “O” and baby is A, B, or AB type, is one of the examples. The RH incompatibility where the mother is Rh-negative and the baby is Rh-positive is another example. I will talk about those situations in detail in my other articles.
Red cells enzymatic defects
Some enzymatic deficiencies may lead to increased destruction of red cells (=hemolysis) and, in turn, to the higher bilirubin production rate. The most common defects are G6PD, Pyruvate Kinase deficiency, and Hexokinase Deficiency.
Structural abnormalities of red cells
Due to genetic defects, erythrocytes (red cells) may be misshaped and undergo faster break down, leading to a higher rate of bilirubin production. Spherocytosis or Eliptocytosis are diseases characterized by the abnormal shape of the red cells.
Infections
Bacterial and viral infection may also cause increased destruction of red blood cells leading to higher bilirubin levels. Usually, infections can be recognized early as patients will be overwhelmingly sick.
Traumatic birth
Traumatic birth resulting in the development of bruises and hematomas will lead to an increased break down of a large number of red cells at once, thus contributing to an increase in bilirubin load soon after the birth.
Jaundice due to decreased elimination of bilirubin
Disorders of elimination will contribute to sustained and increasing bilirubin load in the circulation. Genetic defects such as in Crigler Najjar Disease or hypothyroidism (abnormally low thyroid hormones) affect the amount of conjugating enzymes in the liver, causing impaired elimination of bilirubin from the body.
Jaundice due to increased reabsorption of bilirubin from the gut
Breastfeeding failure jaundice
Breastfeeding failure jaundice occurs during the first week of life when a mother has a hard time establishing effective breastfeeding patterns. It may result in relative starvation, dehydration, and delayed meconium passage (meconium=the first bowel movement that baby passes). That, in turn, will lead to increased reabsorption of bilirubin from the gut back into the circulation, increasing total bilirubin load in the body.
Breast milk jaundice
It usually occurs during the second or third week of life. It is not known why some breastfed babies develop this late jaundice, but it is believed that some ingredients of breastmilk may be causing increased reabsorption of bilirubin from the gut (increase in “enterohepatic circulation”). In some babies, bilirubin levels may reach even 20-30 mg/dl, which may be dangerous for them. Although not widely accepted, one of the therapeutic and diagnostic approaches is stopping breastfeeding for 24-48 hrs and watching a decrease in bilirubin levels.
Disorders of bilirubin excretion from the liver
Due to liver tissue swelling during infection or mechanical-anatomical obstruction, the liver may not be able to excrete bilirubin into the biliary tree and bowel loops. We call this type of jaundice an obstructive type. It leads to direct (conjugated) hyperbilirubinemia. It is sporadic and will not be discussed in this article any further.
What are the risk factors for the development of newborn jaundice?
Risk factors contributing to severe jaundice that will require treatment (hyperbilirubinemia) in a newborn baby:
- Predischarge bilirubin levels in the high risk or high-intermediate risk zone (to determine the risk zone we have to plot bilirubin level on the hour-specific graph developed by Bhutani’s group)
- Exclusive breastfeeding, especially if it is associated with weight loss
- Jaundice that was noticeable in the first 24 hours of life
- Hemolytic disease (increased destruction of red blood cells due to maternal antibodies or cell wall defects)
- Enzymatic deficiencies in red cells (for example G6PD)
- The previous child had significant jaundice
- Cephalhematoma or widespread bruising due to delivery trauma (cephalhematoma is a collection of blood over the baby’s scalp)
- East Asian race
Even if the baby develops severe jaundice that requires treatment with phototherapy or exchange blood transfusion, most of those patients will do well. The following are the risk factors found in patients who developed neurological complications due to severe hyperbilirubinemia:
- Immune hemolytic disease (presence of maternal antibodies in baby’s circulation). More information on this topic here.
- G6PD deficiency
- Asphyxia (low oxygen levels in a baby before and after the birth)
- Sepsis (overwhelming infection)
- Acidosis (elevated amount of acid in the blood)
- Albumin levels in a baby below 3 g/dl
To be clear, the presence of one or two risk factors in a baby does not mean that the baby will have severe jaundice or poor neurological outcomes. These are only statistical associations.
How much jaundice is normal in a newborn baby?
The majority of newborn babies will have some degree of jaundice. Jaundiced skin is a typical and physiologic finding in newborns during the first week of life. That’s why this condition is also called a Physiologic Jaundice or Physiologic Hyperbilirubinemia.
For the full-term babies, physiologic jaundice can be characterized as a rise in bilirubin levels from 2 mg/dl at birth to an average of 6 mg/dl between 2-5 days of life. This peak bilirubin level occurs in white or African-American babies. Newborns of the Asian race tend to have much higher peaks. Subsequently, hyperbilirubinemia resolves within 1-2 weeks after birth and reaches adult levels below 2 mg/dl.
Babies who develop bilirubin levels much higher than the physiologic levels described here are diagnosed with pathologic hyperbilirubinemia or pathologic jaundice. Whenever that is a case, we will try to determine the cause of that exaggerated jaundice and contributing risk factors.
Is jaundice dangerous for newborn babies?
For the vast majority, probably for the 99% babies, jaundice is a benign condition that resolves over time on its own or with phototherapy. In cases where bilirubin rises rapidly to very high levels or baby was discharged home with suboptimal follow up and high levels of bilirubin were detected too late, jaundice may be dangerous and lead to severe neurologic complications and even death.
Retrospective studies of those babies with severe complications showed that usually, culprits were:
- Baby with G6PD (genetic enzyme deficiency)
- Blood type incompatibilities
- Exclusively breastfed baby with significant weight loss without proper follow up
- Parents not having an appointment or missing assigned appointment after discharge
Acute neurologic disease due to bilirubin toxicity is called Acute Bilirubin Encephalopathy (ABE). It is not established yet what level of bilirubin may lead to it. We suspect that prolonged exposure to bilirubin levels exceeding 25-30 mg/dl in a baby older than 48 hrs may result in this syndrome. Historically, Acute Neurologic Encephalopathy used to be known as “Kernicterus.”
The following are early signs of bilirubin encephalopathy:
- Problems with feedings
- Lethargy and changed sleep pattern
- Irritability and difficulty in consoling
- Intermittent arching
- Progressing encephalopathy may lead to baby stopping feeding, seizures, coma, and even death.
Babies who developed bilirubin induced encephalopathy and survived, are likely to develop Chronic Bilirubin-Induced Neurologic Dysfunction (BIND).
The most common features of BIND are:
- Cerebral palsy (choreo-athetoid type)
- Hearing problems (related to both central damage in the brain and the peripheral auditory nerve)
- Abnormal gaze
- Dental hypoplasia (hypoplasia = underdevelopment)
- Cognitive impairment
Children who survived Acute Bilirubin Toxicity and developed Chronic Neurologic Dysfunction will require long term developmental follow up, rehabilitation, and numerous support services.
Epidemiologic studies taught us that the implementation of universal bilirubin screening before discharge home was able to achieve a 40%-70% reduction in the number of babies exposed to bilirubin levels above 25 mg/dl (Potentially dangerous levels for the baby’s brain).
What are the symptoms of jaundice?
The predominant symptom of newborn jaundice is yellowish skin color. Usually, you start seeing yellow skin color first on the face, and in the white areas of the eyes (sclera), later, it spreads in a downward direction covering chest, abdomen, and legs. In the olden days, doctors believed that they could assess the severity of jaundice based only on visual examination of the baby’s skin color. However, data is showing that visual estimations are notoriously inaccurate, and it would be dangerous to rely only on visual examination when assessing newborn jaundice.
Babies who have jaundice due to blood type incompatibility and hemolysis may present with anemia. Thus pale skin may be accompanying finding.
Babies who have very high or extremely high bilirubin levels may have neurological symptoms such as lethargy, poor feedings, abnormal muscle tone, or even seizures. If your baby has such symptoms, it is an emergency, and such a newborn requires immediate medical attention.
In rare situations, when a baby has jaundice due to an obstruction in the liver, the baby may have greenish-yellowish skin color, and its stools may be looking colorless or pale.
How do we diagnose and evaluate newborn jaundice?
Bilirubin levels
As I explained earlier, bilirubin is the chemical directly responsible for jaundice. We can measure the amount of bilirubin in the baby by using two different techniques: transcutaneous (through the skin) and blood test.
The transcutaneous method is non-invasive (does not include any needle prick) and is painless; it provides results immediately. The disadvantage of this technique is that it measures only total bilirubin without differentiating between direct and indirect bilirubin, and it underestimates bilirubin values at higher levels. Additionally, it can not be used after phototherapy has been started.
Blood measurements of bilirubin levels are much more accurate and provide information on both direct and indirect bilirubin concentrations. Once the baby is started on phototherapy, we use only blood bilirubin measurements.
After we obtain bilirubin values, we plot them on the nomograms (graphs developed after observing thousands of babies with jaundice) according to each baby’s age and risk factors. Graphs aid us in deciding whether a patient needs treatment or future follow-up. Depending on risk factors and the so-called “risk zone,” the timing of the repeat bilirubin tests will differ.
Albumin levels
Albumin is a type of protein in the blood to which bilirubin tends to attach. Interestingly bilirubin which is carried by albumins is less likely to cause brain damage. Therefore, the more albumin baby has, the less likely it is to suffer neurological consequences from abnormally high bilirubin levels. Albumin is measured in a blood sample. It is a quick test that most hospitals can do. We do not measure albumin levels in every baby with jaundice. We would measure it only in babies that have bilirubin at the levels close to the point where we would want to consider performing double volume exchange blood transfusion.
Blood type in the baby and mother
All pregnant women have blood type determined during pregnancy, and if it were not done before, it would be done in a labor room. Doctors need to know the mother’s blood type in case there is an emergency: she has post-partum bleeding or needs emergency surgery. Also, knowing the mother’s blood type allows us to find out if the baby is at risk of having blood type incompatibility and, subsequently, a hemolytic reaction.
A hemolytic reaction with jaundice can occur in babies born to mothers with “O” and/or” Rh-negative” blood types and when the baby has A, B, AB, or Rh-positive blood type.
DAT – Direct antiglobulin test (in the past called Coomb’s test)
We do this blood test to find out if there is a reaction between maternal antibodies and baby’s red blood cells. It is needed when the mother and baby have incompatible blood types, as described in the previous section. The test proves that not only the mother and baby have different blood types, but also, there is an ongoing process in the baby’s circulation, causing increased destruction of the baby’s red blood cells. That, in turn, may lead to anemia and jaundice.
CBC – Complete blood count
CBC is a test looking at different types of cells in the blood. It is helpful in cases where there is blood type incompatibility between mother and baby, and there is a hemolytic process confirmed by a positive DAT test. The main values we look at in CBC are numbers of red blood cells and the amount of hemoglobin. These two values tell us if the baby is anemic.
Blood smear
Obtaining a blood smear involves looking at different cells in the blood and their shapes under a microscope. Certain types of blood diseases in which red blood cells are misshaped can lead to hemolysis and increased production of bilirubin. Examples of those blood disorders are spherocytosis or elliptocytosis (red blood cells are in the shape of a sphere or oval).
Measurements of enzymes such as G6PD or Pyruvate Kinase Enzyme.
Deficiencies of some enzymes may contribute to increased or prolonged jaundice. In rare cases where we do not have a precise diagnosis, we can measure those enzymes. We do not perform these tests in every baby with jaundice.
Other tests
There will be rare situations that, after doing most or all the tests mentioned above, we would not have a diagnosis regarding the cause of severe jaundice in a baby. Numerous very specialized tests are available to us, but they are beyond the scope of this article. We can test babies for congenital metabolic diseases, endocrine abnormalities, inherited defects, infections, and many other problems.
How do we treat newborn jaundice?
There are several treatments we can use in the management of jaundice. Treatment will depend on the severity and cause of the disease:
- Phototherapy – the most important
- Nutrition and Hydration
- Immunoglobulin infusion
- Double volume exchange blood transfusion
- Supplemental blood transfusion
- Phenobarbital
Phototherapy
Phototherapy with proper nutrition and hydration is the most important treatment modality of clinically significant jaundice. Phototherapy utilizes narrow-spectrum lights and works by transforming bilirubin into soluble compounds that can be excreted from the baby’s body. Due to the significant role phototherapy plays in the nursery and many questions parents always have about it, I wrote another article focused entirely on that subject. You can access it here.
Proper nutrition and hydration
Nutrition and proper hydration are essential. That will ensure the uptake of bilirubin by the liver and kidneys, which participate in its excretion. In addition to that, intestinal peristalsis and frequent stooling will contribute to decreased reabsorption of bilirubin from bowel loops, thus reducing the total bilirubin load in the body.
Immunoglobulin Infusion
Immunoglobulin infusions may play a role in hemolytic jaundice due to blood type incompatibilities. (ABO or Rh incompatibility). The exact mechanism of its effectiveness is unknown. We theorize that immunoglobulins may be able to block sites on a baby’s red blood cells to which maternal antibodies would want to attach to cause their breakdown. Preventing the destruction of the baby’s red blood cells will contribute to decreasing the final bilirubin load, which is responsible for neonatal jaundice.
Immunoglobulins could be indicated for babies with significant immune-hemolytic jaundice where bilirubin levels are 2-3 mg/dl below exchange transfusion levels. We use immunoglobulins (IgG) to avoid exchange transfusion, which is considered a more aggressive therapy.
Usually, IgG infusion is tolerated very well, but sometimes babies may have rare side effects such as low blood pressure (hypotension), fast heart rate (tachycardia), and allergic reactions. To decrease the likelihood of adverse reactions, we infuse immunoglobulins over several hours and monitor the baby’s vital signs closely (temperature, respiratory rate, heart rate, and blood pressure).
Double volume exchange blood transfusion
When bilirubin is rising extremely fast, or it is at the level likely to cause neurological damage, exchange transfusion is indicated. For the procedure, we request blood from the blood bank that is compatible with the baby’s blood and does not contain any antibodies against the baby’s red blood cells.
Typically, the procedure is performed using one or two centrally placed umbilical catheters (An umbilical catheter is a small sterile plastic tube inserted into the umbilicus and connected to a syringe, IV bag, or bag containing the blood). During the procedure, we will be removing small amounts of the baby’s own blood and replacing it with new blood obtained from the blood bank. The goal is to replace the double volume of the baby’s blood achieving a significant decrease in bilirubin levels.
The following risks that are associated with giving blood products can occur during this procedure:
- Allergic reactions
- Blood pressure changes
- Infections
- Fever
- Thrombosis – clots
- Thrombocytopenia
Specific adverse reactions that can happen in newborns after double volume blood exchange transfusion include:
- Apnea (pause in breathing)
- Bradycardia (low heart rate)
- Cyanosis
- Vasoconstriction – vasospasm
- Thrombosis in blood vessels or around the catheter
- Necrotizing enterocolitis (a severe inflammatory disease of the bowels, more common in premature babies)
- Death – very rare but described in the literature
Nowadays, we don’t perform exchange transfusions very often. It is thanks to very effective phototherapy lamps and the availability of IgG for hemolytic jaundice. Only some hospitals are capable of performing this complicated procedure; therefore, if your baby needs it, doctors may have to transfer your baby to another institution.
Supplemental blood transfusion
Supplementary blood transfusion is not a jaundice treatment per se, but it may be needed in hemolytic jaundice when the disease is also accompanied by anemia. Hyperbilirubinemia due to blood type incompatibilities (ABO or Rh) may be associated with severe anemias requiring red blood cell transfusions. (Of note, we rarely transfuse whole blood). For the treatment of anemia, we would be giving so-called PRBCs = Packed Red Blood Cells.
Stopping breastfeeding for 1-2 days (controversial)
Some babies may have breastmilk jaundice. It is a disease due to some unknown factors present in breast milk. Occasionally, when doctors are not sure about the reasons for jaundice or want bilirubin to decrease, they may recommend stopping breastfeeding for 24-48 hours. If bilirubin decreases, it confirms their presumptive diagnosis of breast milk jaundice. This approach is somewhat outdated and controversial, however still in use by some providers.
Phenobarbital
Phenobarbital is a medication known for its use in controlling seizures in children. Its use in the treatment or prevention of jaundice is less known. Phenobarbital can stimulate the activity of liver enzymes that are involved in the transformation and excretion of bilirubin out of our body.
It can be useful in some congenital enzymatic defects (Crigler Najar disease) or occasionally in cholestatic jaundice in premature babies.
What is the prognosis for newborn jaundice?
The discussion here pertains mainly to non-obstructive and unconjugated jaundice (hyperbilirubinemia), which constitutes the vast majority of cases with jaundice disease in the nursery.
60%-70% of newborn babies after birth have visible jaundice. The majority of them do not need any intervention. The newborn baby’s body resolves it on its own. Probably less than 10% of babies with jaundice will need phototherapy. Again, the majority of those babies treated with phototherapy will be fine.
Among babies with hemolytic jaundice, particularly the ones due to ABO or Rh incompatibility, some babies will require IgG infusion, exchange blood transfusion, or supplemental blood transfusion. Most of them will recover fully without any sequelae.
Very few babies will have the most severe form of jaundice that progressed very quickly or reached extremely high bilirubin levels that become toxic to the baby’s brain. These conditions are called Acute Bilirubin Encephalopathy and chronic disease called Chronic Bilirubin Induced Neurologic Dysfunction (BIND).
The incidence of acute bilirubin-induced toxicity to the baby’s brain is probably about 1 in 30 000 – 1 in 70 000 healthy newborn babies.
Can a baby die from jaundice?
For most babies, jaundice is a benign condition that will go away after 7-10 days. Unfortunately, few babies may have very quickly progressing jaundice with extremely high bilirubin levels leading to neurological sequelae and even death. Researchers estimate that approximately 1 out of 30 000 – 70 000 babies may develop a severe neurological syndrome called Acute Bilirubin Encephalopathy (ABE), and about 10% of babies with ABE may die. (Source article).
Nowadays, those cited statistical numbers may be lower because almost all pediatricians and neonatologists across the United States implemented very close monitoring of bilirubin levels after birth. In addition to that, we screen mothers and babies for any blood type incompatibilities (ABO and Rh). If detected, we tend to follow up with bilirubin levels much earlier than we would do in other babies who are not affected.
Can I continue breastfeeding a baby with jaundice?
It is essential to continue breastfeeding every baby with jaundice. Frequent and of adequate volume feedings will promote intestinal peristalsis (contractions and movements of bowel loops), thus decreasing the time the bowel contents stay in the same place. This action will also reduce the reabsorption of bilirubin that has already been excreted by the liver into the bowel loops.
Proper hydration, feedings, and bowel movements will contribute to a quicker resolution of jaundice in most babies. If a mother has a difficult time establishing breastfeeding, the baby is dehydrated, and has clinically significant jaundice, supplementation with formula, or starting IV fluids may be necessary.
What questions should I ask if my baby has jaundice?
- What is the cause of jaundice?
- Does my baby need treatment?
- If the baby is already on phototherapy, do you expect that other treatments such as immunoglobulin or exchange blood transfusion may be needed?
- How close are current bilirubin values (bilirubin levels are a measure of severity of jaundice) to levels at which the exchange blood transfusion would be needed?
- Can phototherapy be administered in the rooming-in room or baby must be taken away from me to the nursery?
- Can I continue breastfeeding?
- How can I help my baby, who is under phototherapy?
- When are you planning to do another bilirubin level?
- When do you expect my baby to be ready for discharge home?
- If you think that baby may need immunoglobulin infusion or exchange transfusion, do you have the capability to do it here, or my baby will be transferred to another institution?
- After discharge home, will I have to bring my baby to a pediatrician to recheck bilirubin levels?
You can read my comprehensive article on Phototherapy for Newborn Jaundice here.
Disclaimer:
This article is only for general information purposes. It should not be viewed as any medical advice. There is a chance that the information here may be inaccurate. It would be best if you always discussed all health-related matters with your doctor before making any decisions that may affect your health or the health of your family members.