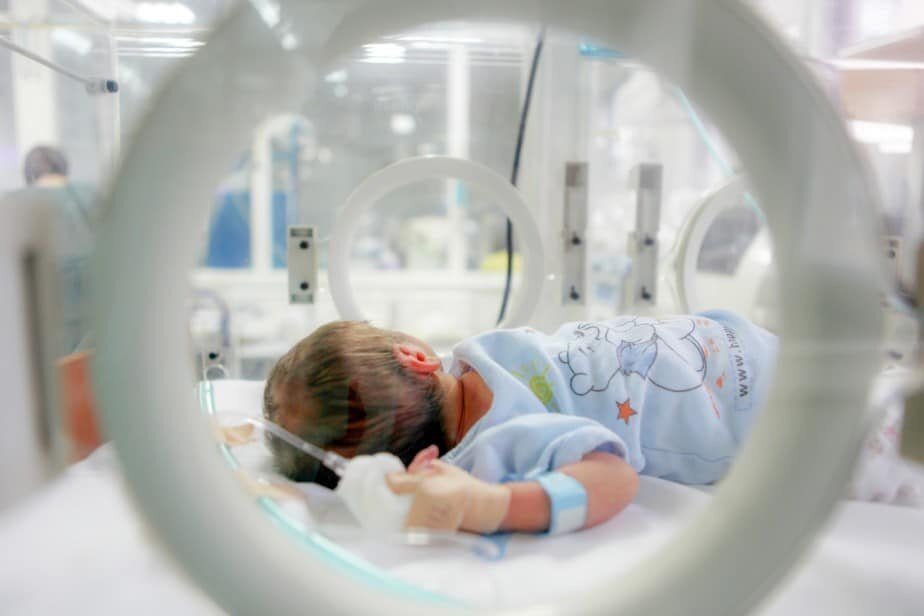
Premature birth is defined as birth before completed 37 weeks of gestational age and is quite common in the USA (Source). Rates of prematurity depend on the race and range between 9% for white babies to 14% for black babies. It is not surprising that parents and families are very interested in learning how do we treat premature babies in the hospital.
How are premature babies cared for?
- Provision of a neutral thermal environment
- Tube feedings and IV fluids
- Respiratory support
- Medications: surfactant, antibiotics, caffeine, indomethacin or ibuprofen
- Routine measures such as Hepatitis B vaccine, Vitamin K, Erythromycin eye ointment
Every premature baby will be having a unique set of problems and challenges that will have to be addressed by its doctors. However, it would be safe to say that almost all babies born at less than 32 weeks of gestational age will be treated using all modalities of treatment mentioned above. I will explain “why” and “how” about each therapy below.
However, If you have a premature baby born before 32 weeks receiving treatment in the NICU right now, I encourage you to explore also my book “Babies Born Early“
Providing an appropriate thermal environment
The majority of premature babies are not able to maintain normal body temperature after birth. Many times this problem is the last one that gets resolved before a baby can be sent home. Often, the baby gained enough weight, can eat well by mouth without any difficulties, resolved all breathing problems, but still needs to be in the isolette to stay warm.
Preemies get cold because:
- small body weight and a thin layer of skin and fat
- immature brain not able to regulate temperature well
- inadequate amount of energy sources in the body
- metabolic immaturity
Premature babies staying in NICU who have problems with body temperature will be placed in isolettes or on radiant warmer beds.
The radiant warmer is a small table with a mattress on it, and a heat lamp placed above. We use it right after delivery and during the first few hours of life. The main advantage of it is that it allows several people to have unrestricted access to the baby. Therefore, it is used for the stabilization after birth and to perform all the necessary procedures.
Isolette is a more permanent solution. It is a plastic box in which we blow warmed and humidified air. The amount of heat is regulated automatically by a computer and adjusted to the baby’s needs. Babies are kept in isolettes until they are ready to come out to open crib, usually close to their discharge home.
Some people use another term for isolette: incubator.
Feedings and fluids
Process of feeding requires three separate physiological functions to be developed and coordinated well:
- sucking
- swallowing
- breathing
Maturation of feeding skills usually starts around 32-34 weeks of gestational age and sometimes is not completed even until 38 weeks of corrected gestational age. It is not unusual to see even some of the early term babies (born at 37 weeks and a few days) having feeding problems.
When a premature baby is very sick, we can provide fluids and all necessary nutrients intravenously. If we expect that baby will need intravenous nutrition for a long time, we would have to insert special types of intravenous catheters called central lines.
Veins in babies are very tiny, and maintaining regular IV access beyond several days is a challenging task, if not impossible, thus need for central lines.
Premature babies are started on tube feedings as soon as they are stable. The tube feedings are also called gavage feedings or NG/OG feedings. A nurse will insert a small, flexible plastic tube through the nose or mouth directly into the stomach. After that, she will connect a syringe with breast milk or formula, and the milk will be delivered directly into the baby’s stomach.
If the baby is around 32 weeks of gestational age and is showing interest in oral feedings, a nurse will attempt bottle feeding first, and then she will deliver the remaining amount of milk through the tube.
Respiratory support
The vast majority of premature babies develop breathing problems after birth for which they need to be treated in NICU. Newborn babies may suffer from different respiratory problems such as Respiratory Distress Syndrome, Bronchopulmonary Dysplasia, Transient Tachypnea of Newborns, or Pneumonia. I wrote separate articles focusing on those conditions, and you can find them here.
In general, the type of respiratory support does not depend on the particular disease; it rather depends more on the severity of the respiratory problem.
Oxygen therapy
Many babies with breathing problems need additional oxygen to maintain appropriate oxygen levels in the body. Room air has 21% oxygen. However, if required by the baby, we can provide up to 100% oxygen.
Supplementary oxygen can be provided using oxy hood, nasal cannulas, CPAP devices, or ventilators.
Supporting breathing
If the baby has increased work of breathing or stops breathing for periods of time, we need to support its breathing using various techniques.
Oxyhood – it is a plastic box that surrounds the baby’s head. We can blow air with supplementary oxygen into it to increase the availability of oxygen to the baby. Nowadays, it is not used that much for premature babies.
Nasal cannulas – plastic tubing that is placed in the baby’s nose. It provides an increased flow of the air-oxygen mixture. We use it only for very mild respiratory diseases.
CPAP device – delivers a flow of the air-oxygen mixture with the addition of extra airway pressure during the expiratory phase of breathing effort. While on CPAP, the baby is still breathing entirely on its own. This technique is used for moderately sick premie babies.
Ventilator or breathing machine – It is used for the most severely sick newborns. The breathing machine can support the baby’s breathing effort or provide all necessary external breaths for the baby. It can also offer supplementary oxygen as needed for the baby. In order to place the baby on the ventilator, a doctor will have to put a breathing tube in the baby’s windpipe and connect that tube to the machine.
What are the most common medications used in premature babies?
We do not use many medicines to treat premature babies. The reason for that is that the main reason premature babies are sick is their physiologic immaturity. Unfortunately, there is no medication capable of speeding up the maturity of all organs in the baby. Therefore, during the NICU stay, doctors mainly support maturation processes in a baby by maintaining physiologic functions; we do not treat any particular sickness per se.
Below, I described a few medications that we do use in NICU.
Antibiotics (Ampicillin and Gentamicin)
Infection in a mother may be a cause for premature delivery, and subsequently, the baby may be infected. It is common practice to treat sick premature babies after birth with antibiotics (most commonly with Ampicillin and Gentamicin) while waiting for results of blood tests that would tell us if the baby indeed had an infection or not.
Since many babies undergo various invasive procedures, they are at risk for acquired infections during their NICU stay. Any sudden deterioration of the general condition in a baby may be the first sign of such a disease. Hospital-acquired infections are also treated with antibiotics.
Caffeine
The majority of premature babies that were born before 32 weeks of gestational age will develop apnea of prematurity. Apnea is a condition where the baby “forgets” to breathe for 10-20 seconds. Caffeine, which is a chemical substance also found in tea and coffee, is the drug of choice to treat Apnea of Prematurity.
Surfactant
Respiratory Distress Syndrome (RDS) is the most common respiratory disease in babies born at less than 32 weeks of gestational age. This condition is due to anatomic and chemical immaturity of the lungs. Lungs in this disease lack a chemical substance called surfactant. Surfactant prevents distal portions of the lungs from collapsing.
Fortunately, scientists were able to extract surfactant from animals and synthesize it in a lab. We can administer Surfactant to sick newborn babies with RDS. To deliver surfactant to the baby, we have to place a breathing tube into the baby’s windpipe. We inject Surfactant via that tube directly into the baby’s lungs.
After the administration of the surfactant, babies are placed on the CPAP device or ventilator.
Indometacin or Ibuprofen for treatment of PDA
The cardiovascular system of the fetus differs from one of the newborn babies. Immediately after the birth of the baby, specific changes should take place in the circulatory system. In some premature babies, those processes do not take place, and some blood vessels that should stop functioning and get closed, still function and create problems for the baby.
One of these conditions is called Patent Ductus Arteriosus. Ductus Arteriosus is a vessel that should stop functioning in a baby after birth, and sometimes it does not.
PDA may contribute to blood pressure problems or breathing problems in a baby; therefore, sometimes, it needs to be treated. We can treat PDA medically with Indomethacin or Ibuprofen. If the baby does not respond favorably to the medication, surgery may also be an option.
Phototherapy
Jaundice or hyperbilirubinemia is probably the most common condition occurring in both full-term and premature babies. You can find on my website several articles I wrote on this topic.
Some babies need therapy for jaundice, and those babies will be started on phototherapy. Phototherapy is a light therapy that changes properties of bilirubin (bilirubin is a culprit in jaundice disease) in the baby’s skin, allowing for its faster excretion from the body.

Baby under phototherapy
Routine measures (after birth and before discharge)
Just because a baby is born premature, it does not mean we can forgo all preventive measures that are offered to full-term babies. Depending on the gestational age and birth weight of the baby, the following procedures will be provided to most premature babies:
- Vitamin K after birth- to prevent bleedings
- Hepatitis B vaccine – to prevent Hepatitis B viral disease
- 2 months’ vaccinations if the baby is still in the NICU
- EYE Erythromycin ointment right after birth- to prevent Gonococcal infection in the baby’s eyes
- Car seat test before the discharge home
- Hearing test before the discharge home
There is a lot of interesting facts that one can learn about premature babies and how we care for them. I would like to encourage you to read an article in which I talk more about prematurity and different terms used to describe premature babies.
If you are interested to learn more about NICU and people working there, start reading here.
Disclaimer:
This article is only for general information purposes. It should not be viewed as any medical advice. There is a chance that information here may be inaccurate. It would be best if you always discussed all health-related matters with your doctor before making any decisions that may affect your health or health of your family members.